What is diverticular disease?
Diverticular disease consists of three conditions involving ‘diverticula’: diverticulosis, diverticulitis and diverticular bleeding.
Diverticula
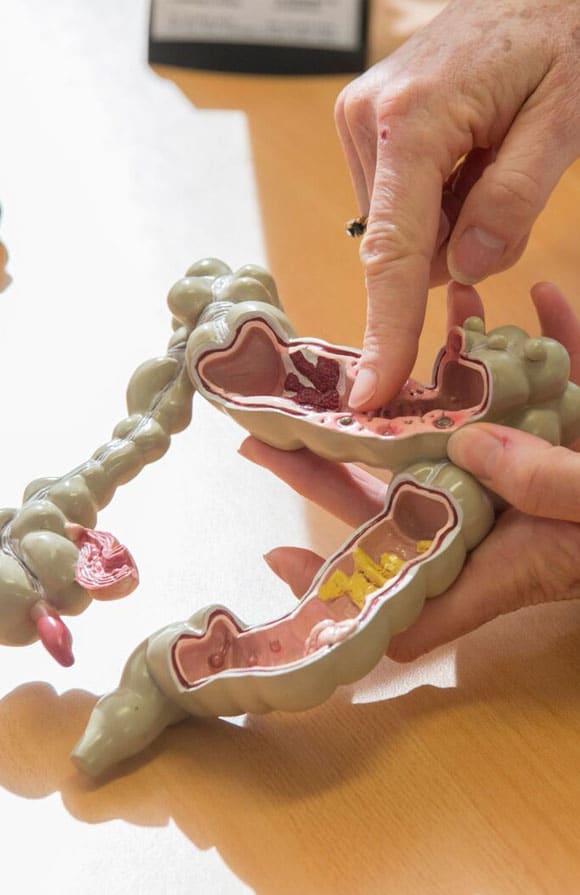
Diverticula are small, bulging pouches that stick out of the side of the intestinal wall. They can occur anywhere in the digestive tract, but they are most common in the colon.
Diverticula form due to increased pressure on weak spots along the intestinal walls. The colon often becomes weaker with age and with pressure from straining to pass stools.
Diverticulosis
If you have diverticula but no symptoms, you have diverticulosis. This is very common. By age 40, about 10% of people have diverticulosis and by age 60, about 50% of people have developed diverticula.
Often diverticulosis is often found when you’ve had a test (e.g. colonoscopy) for something else.
About one in 5 people with diverticulosis go on to develop symptoms.
Diverticulitis
Diverticulitis means one or more of your diverticula are inflamed or infected. This is usually because the diverticula become blocked with faecal matter. Around 25% of people with diverticulitis develop complications and may need surgery.
Complications include:
- abscess formation
- perforation – this may allow bowel contents to leak into the abdominal cavity. This is a medical emergency
- peritonitis – this may occur after perforation. Bacteria in the bowel contents can infect of the lining of the abdominal cavity. This may be life threatening
- bowel obstruction.
Diverticular bleeding
This happens when small blood vessels around the diverticula are damaged.
What are the symptoms of diverticular disease?
Diverticulosis symptoms
Diverticulosis does not usually cause symptoms.
Diverticulitis symptoms
Symptoms of diverticulitis include:
- painful cramps or tenderness in the lower abdomen
- bloating
- diarrhoea or constipation (or alternating between both)
- nausea or vomiting
- fevers or chills.
Diverticular bleeding
Diverticular bleeding is usually painless. You might see bright red or maroon blood with bowel motions. Occasionally the bleeding can be severe.
These symptoms are not exclusive to diverticular disease. It’s important to tell your doctor about your symptoms. This ensures that you get the right diagnosis and the right treatment.
What causes diverticular disease?
The major factor leading to diverticular disease is getting older.
Diverticular disease specialists generally think a combination of genetics and diet cause diverticular disease.
Western people with a low-fibre diet seem to be most at risk.
How is diverticular disease diagnosed?
Diverticulosis has no symptoms, so it tends to be found when looking for other conditions such as colorectal cancer.
Diverticulitis is usually diagnosed during an acute attack. Tests to diagnose diverticular disease include:
- medical history – such as diet
- physical examination – including digital rectal examination where your doctor inserts a gloved, lubricated finger into the anal canal and feels for anything abnormal
- colonoscopy – where a thin flexible tube is inserted into your anus so that your diverticular disease specialist can look at your large intestine
- Gastrografin enema – this is where X-rays are taken after a special contrasting dye (Gastrografin) is flushed into the bowel via your anus
- CT scan – to detect abscesses outside the bowel lining
- blood tests – to check for signs of infection
- faecal testing – looking for blood in the faeces or infections that can mimic the symptoms of diverticulitis.
How is diverticular disease treated?
Diverticulosis
If you have diverticula without symptoms, you do not need special treatment. But you should consider increasing the fibre in your diet. This may prevent new diverticula forming, diverticulitis or diverticular bleeding.
People with diverticulosis used to be told to avoid seeds and nuts because of their potential to lodge in the diverticula. This is no longer the case.
Diverticulitis
Treatment depends on the severity of your symptoms.
If you have mild symptoms, your diverticulitis specialist may recommend a clear liquid diet and oral antibiotics. You might need some pain relief.
If you develop one or more of the following symptoms, you may need more intensive treatment:
- fever (temperature above 38ºC)
- severe or worsening abdominal pain
- inability to hold down fluids.
About 85% of people will get better with medical treatment, while around 15% need surgery.
You will probably need surgery if you develop a perforation, peritonitis or bowel obstruction. You might also need surgery if your attack of diverticulitis doesn’t resolve.
Diverticular bleeding
Most cases of diverticular bleeding settle down on their own. Some people will need treatment to stop bleeding. This may involve a colonoscopy, angiography or surgery.
Your diverticular disease specialist will talk to you about the best treatment for you.
